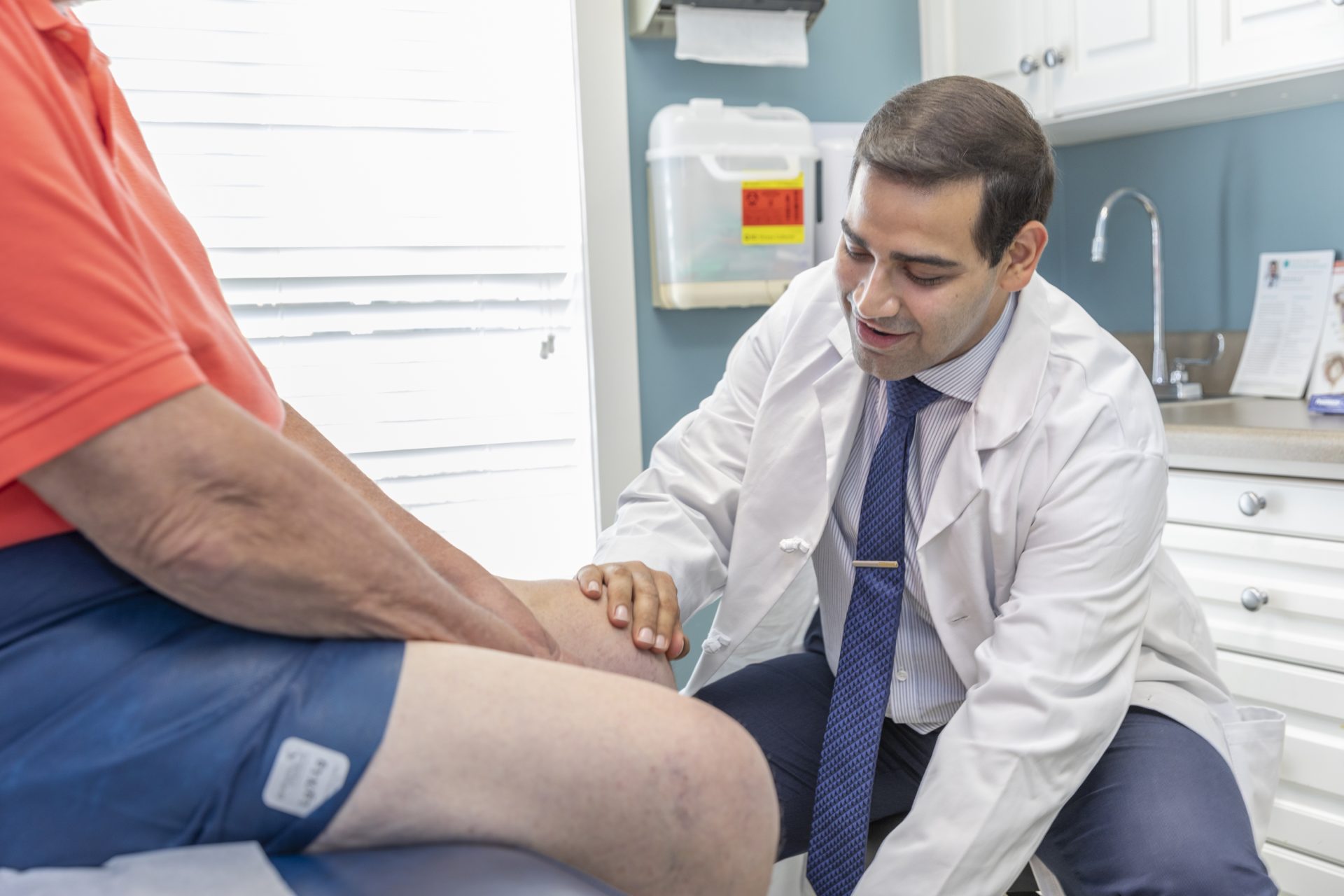
A recent nationwide study by Johns Hopkins Medicine researchers revealed women younger than 65 are dying from heart disease at an increased rate compared with past years.
It’s no secret that women tend to put the health of others before their own, especially those who must care for children, manage a household, work full time and shoulder other responsibilities. So, it may not be surprising that a recent nationwide study by Johns Hopkins Medicine researchers revealed women younger than 65 are dying from heart disease at an increased rate compared with past years.
“Young women in the United States are becoming less healthy, which is now reversing prior improvements seen in heart disease deaths for the gender,” says Erin Michos M.D., M.H.S., director of women’s cardiovascular health and associate professor of medicine at the Johns Hopkins University School of Medicine. “In a previous study in December 2018, we showed that more attention should be paid to the health of young women, particularly those with the risk factors that contribute to heart disease.”
“Our latest research confirms that need still exists,” she says.
In the new study—an analysis of U.S. death certificates between 1999 and 2018 from a national database—Michos and her colleagues compared heart disease and cancer deaths in women under 65. Their findings were reported Feb. 8, 2021, in the European Heart Journal – Quality of Care and Clinical Outcomes.
The researchers found that overall during the 10-year study period, cancer was the most prevalent cause of premature death in women under 65—slightly more than twice as much as heart disease. However, the overall cancer mortality rate (age adjusted) for women under 65 decreased from 62 to 45 deaths per 100,000 people while the overall heart disease mortality rate (age adjusted) dropped from 29 to 23 deaths per 100,000.
Another finding from the study was that the annual percentage change (APC) in age-adjusted mortality rates for cancer declined year after year during the study period, while it increased for heart disease in two specific groups from 2010 to 2018: women 25 to 34 (2.2%) and women 55 to 64 (0.5%). The APCs rose significantly after 2008 for women living in the midwestern United States, medium and small metropolitan areas, and rural areas. Additionally, APCs were found to have increased for white women from 2009 to 2013 and for Native American women from 2009 to 2018.
Finally, the researchers determined the mortality gap between cancer and heart disease in women under 65 narrowed from a mortality rate (age adjusted) of 33 deaths per 100,000 in 1999 to 23 deaths per 100,000 in 2018.
Compounding the problem of premature death from heart disease in women under 65, say the researchers, is the commonly held misconception that women are not at risk for heart disease before menopause. But in fact, statistics show one-third of all heart issues in women occur before age 65.
Another major factor—the gender gap in cardiac disease care—was revealed in the 2018 study by Michos and her colleagues.
“We showed that women were not getting the same level of care as men, and they feel that way too. Women are more likely to report communication problems with health care providers and dissatisfaction with their health care experience, and we think this contributes to the disparities that we see when it comes to getting preventive and other treatment for cardiovascular disease,” said Michos after the 2018 study was published.
Along with advocating for equal health care, Michos recommends that women combat the risk of premature cardiac death by eating a healthy and balanced diet, getting regular physical activity, not smoking, and maintaining healthy blood pressure, blood sugar, cholesterol level and body weight.
Source: https://www.hopkinsmedicine.org/news/newsroom/news-releases/research-story-tip-heart-disease-gaining-on-cancer-as-a-major-cause-of-death-in-young-women-say-researchers
Exclusive content from CARE Magazine